Partnering with Faith-based Organizations to Achieve Health for All
March 19, 2019 | 4 Minute ReadFaith-based organizations deliver more than 30 percent of health services across sub-Saharan Africa, according to the Africa Christian Health Associations Platform. Without meaningful engagement with this community, we jeopardize our pursuit of health for all.
To achieve health for all, the global health community needs the participation of everyone working in the health system: public, private, or not-for-profit. Often global health programming focuses on public sector health systems. But, by some accounts, faith-based organizations deliver between 30 and 70 percent of health services across sub-Saharan Africa. To provide equitable and accessible health services for all, a local systems approach should include public-private partnerships that integrate faith-based health systems.
Ambassador-at-Large and U.S. Global AIDS Coordinator Deborah Birx has noted that communities of faith “have unique health care delivery capacities and deep relationships of trust with individuals and families in need, both of which are vital to helping us achieve our goals.”
At the recent Africa Christian Health Associations Platform Biennial Conference in Cameroon, colleagues and I shared our experience partnering with the Christian Health Association of Malawi (CHAM) to strengthen the country’s health workforce through the USAID HRH2030 program. We also learned more about how to productively collaborate with faith-based organizations in sub-Saharan Africa to provide equitable, accessible, available, affordable, and high-quality health services.
Here are four key takeaways:
1. People-centered care is critical for reaching health goals.
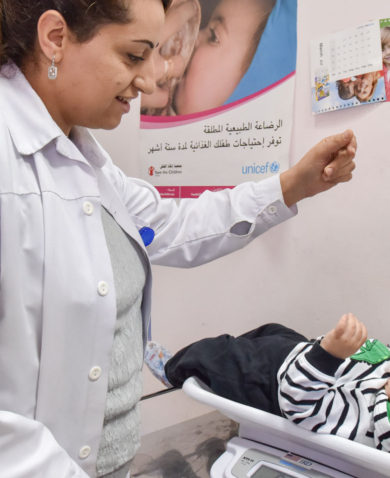
Critical to quality and equitable health services is compassionate and people-centered health care. Faith-based organizations have historically recognized the centrality of putting people first to truly address health issues. The international community can learn from the trust and accountability that faith-based organizations have within communities and their holistic approach to delivering health services. Faith-based organizations frequently excel at linking the community to both health services and social welfare services in a way the public sector consistently finds challenging. Faith-based organizations set an example of prioritizing people-centered care, frequently protect vulnerable groups and people with disabilities, and are skilled in reaching those who traditionally do not seek services such as men and youth. Further, faith-based organizations often are located in poor, remote areas and fill a gap often not met by public sector health services. We can learn from these organizations’ ability to reach more people with health services and collaborate with them to support a fully functioning health system that serves all people.
2. Faith-based organizations don’t always have a seat at the table.
In a charged moment of the conference, attendees tackled the question of why faith-based organizations are often not invited to technical, planning, and policy meetings in the same way as public sector officials and international partners. This highlights a trend where the global public health community has often neglected to involve faith-based organizations. However, the landscape is slowly shifting with PEPFAR’s declaration to reach a benchmark of directing 70 percent of funding to “indigenous” organizations — those based in the countries in which they operate — by the end of Fiscal Year 2020. Moreover, PEPFAR recently announced that it will invest $100 million to address key gaps toward achieving HIV epidemic control by leveraging the unique capacities and compassion of faith-based organizations and communities. These entities provide a substantial proportion of health services, especially in countries with weak health systems or that are post-conflict.
3. The focus has been on service delivery, not management and administration.
Faith-based organizations have limited resources and tend to use them to maximize delivery of health services. As a result, they often have some technical, financial management, compliance, reporting, and communications capacity gaps to address in preparation for potentially increasing levels of donor funding. As USAID and PEPFAR prioritize funding local organizations, and faith-based organizations specifically, they must recognize and invest time and resources to build management capacity. On the technical front, it is vital to emphasize equity in service delivery to ensure no one is left behind, including vulnerable groups who may not fit into traditional religious norms, such as the LGBTQ community or women seeking family planning options before marriage. Experienced international development professionals and partners are needed for capacity development and mentorship during this time of transition.
4. If you want to go fast, go alone. If you want to go far, go together.
It is better to include faith-based organizations and align messages — particularly when it comes to serving key populations — rather than remain fragmented, which could exacerbate harmful cultural norms. For example, early in the HIV epidemic, getting faith leaders engaged was challenging, but, once involved, the faith community became powerful leaders in promoting messages about HIV, particularly the ABCs of abstinence, be faithful, and condoms. After years of work and studies on behavior change communication, researchers found that the ABCs were not effective for controlling the epidemic. However, promotion of the ABC’s had an ancillary effect on overall stigma reduction because people were talking about HIV, and it was present in the media. In moving away from the ABC messaging, HIV programs often stopped engaging with faith leaders, contributing to a resurgence of stigma in many places. The ability of faith-based organizations to counter stigma and discrimination is critical in reaching epidemic control and is essential to strengthen the alignment of faith-based organizations with national systems and priorities.
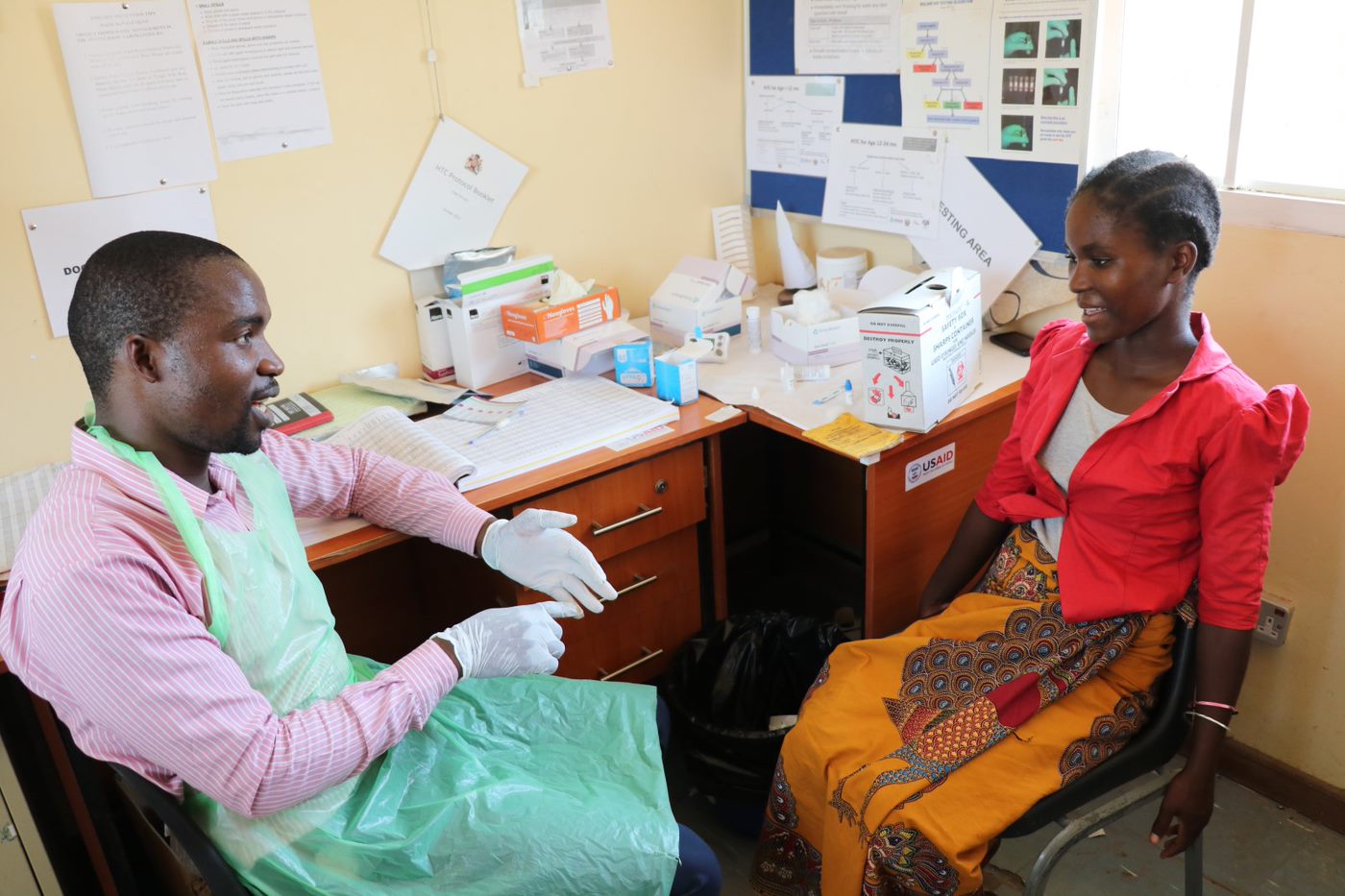
To achieve health for all, we believe the global health community needs to thoughtfully and deliberately engage faith-based organizations. On HRH2030, we partner with the CHAM to jointly support health workers to address shortages in HIV service delivery. Our partnership reflects some of the key takeaways above. We take a people-centered approach by working together with CHAM to recruit high-quality health workers in high-HIV burden facilities. We facilitate closer collaboration between CHAM and the Government of Malawi to help CHAM get a seat at the table. We provide capacity development support to CHAM on management and administration, so they are well prepared to work with donors and other stakeholders. And, we work with CHAM on health systems strengthening activities. The future health system that achieves health for all must include the public and private sectors and consider the unique challenges and opportunities faith-based health systems hold for improving health outcomes.