3 Questions with Samantha Law on the Importance of Creating a Gender-Competent Health Workforce
April 19, 2018 | 3 Minute ReadHealth workers are not immune to gender bias and this can affect the care they provide to patients. How can we give health workers the knowledge and skills they need to provide equitable care to all?
This post was adapted from one that originally appeared on the USAID Human Resources for Health in 2030 (HRH2030) program’s website. Samantha Law is a manager with Chemonics’ Global Health Division and serves as gender lead on USAID HRH2030.
People and organizations work daily to augment the voices and rights of women around the globe. There is a continued need to strive for gender equality — the absence of discrimination on the basis of a person’s sex. USAID’s Human Resources for Health in 2030 (HRH2030) program is fully on board, working toward a world in which everyone has access to the acceptable, high-quality health workforce needed for a healthy, productive life regardless of their sex. While countries continue to make progress in health workforce development, the need to increase health providers’ awareness of gender and foster skills necessary to provide gender-equitable health care remains. This is particularly true for family planning, where access to a full range of information and services can be affected, often unintentionally, by provider gender biases.
Why is defining and advancing gender competence in the health workforce, particularly for family planning, so important?
Gender — how a society ascribes day-to-day roles, rights, and responsibilities to women and men —affects access to information and services in the health sector, particularly in family planning and reproductive health. Decisions about if, when, and how to start a family or follow through on a chosen family planning method are intrinsically tied to ever-changing gender norms and roles. For instance, traditional gender norms that assign a man as the decision-maker for the household may constrain a woman’s ability to make decisions about her reproductive health. Likewise, because of socially-constructed roles and relationships, health providers operate with their own gender biases when delivering family planning services, which can lead to different treatment of women, men, girls, and boys. For example, a provider might perpetuate inequitable gender roles by not providing contraception to a married adolescent girl. In another instance, a provider might withhold information about long-acting contraceptive methods from a client if she has not had a child yet because of a socially-ascribed necessity for her to fulfill her role as a mother. In other words, gender norms and biases can impact health providers’ ability to deliver high-quality health care and information.
With gender competence, a health worker is aware of how gender may influence clients’ ability to exercise their reproductive intentions. As a result, a health worker can contribute to creating a safe and secure space for questions, discussion, and informed choice. Also, with gender competence, a health worker is aware of his or her own need to overcome biases to provide equitable, high-quality services and meet his or her clients’ reproductive health needs. Gender competence will reinforce gender equality both within and beyond health service delivery and will contribute to positive health outcomes overall!
How is your work with HRH2030 aiming to create a more gender-competent workforce?
It’s critically important for the health workforce to have gender competence to deliver accessible, available, acceptable, and high-quality health services. Thus, HRH2030 is working with USAID’s Office of Population and Reproductive Health to link gender competence and family planning through a global standard definition of gender competence and a competency framework that delineates the knowledge, skills, and attitudes a gender-competent family planning provider should demonstrate.
While still in draft form, our framework requires the improved capacity of providers to:
- Promote clients’ individual agency
- Engage men and boys as partners and family planning users
- Facilitate positive communication and cooperative decision-making by couples
- Utilize gender-sensitive communication
- Address gender-based violence
- Support legal rights and status
A provider who supports a client’s legal rights and status, for example, should know the local laws and policies regarding consent to engage in sexual activity and if a partner’s permission is legally required for the client to access family planning services. The provider should then have the capacity to respond to the needs of the client to help her or him make voluntary and informed decisions about family planning. The draft graphic below shows how these concepts interact to lead to improved reproductive health outcomes and increased gender equality.
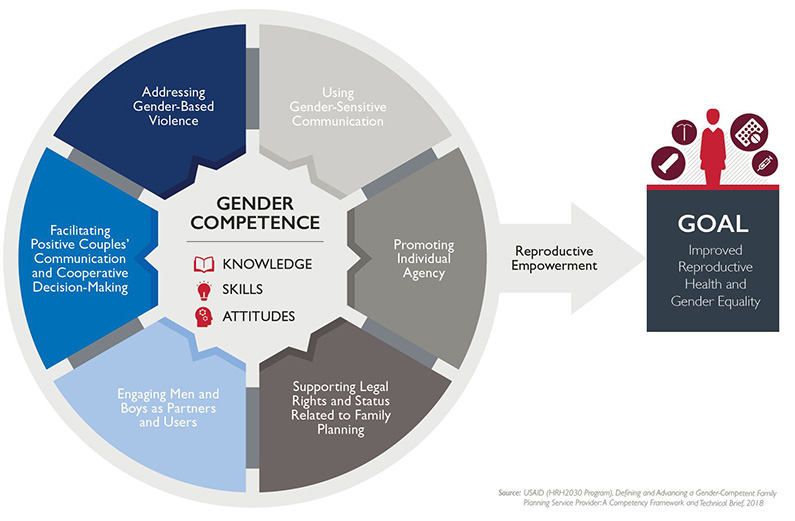
Where are you in this process? What are the next steps?
HRH2030 is in the development and validation stage of our work to define gender competence and create the competency framework. As part of this, we have worked with gender, family planning, and human resources for health experts to provide input and peer review for the work. Our next step is to test the competencies with frontline family planning providers to validate if they are relevant and comprehensive, as well as add contextualization to help with understanding and adaptation. Ultimately, we’d like to streamline the concepts into pre-service education curricula so that learning about gender is inherent in learning about family planning service delivery. We believe that increasing gender competence among this health workforce will lead to greater gender equality.