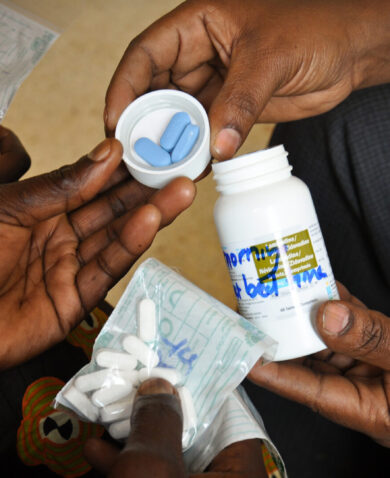
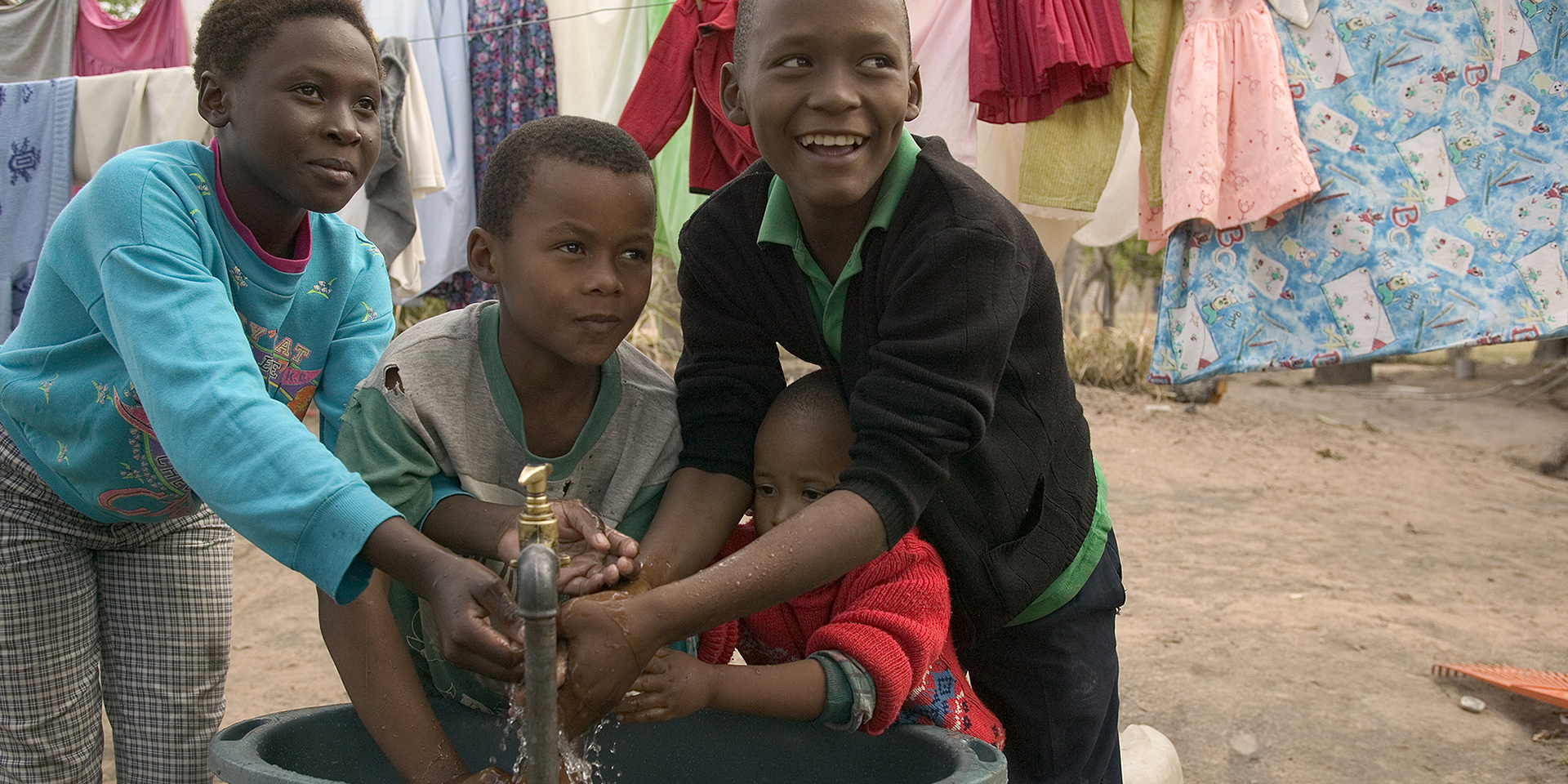Official reports grossly underestimate the burden of cholera and, exacerbating the problem, many country health systems are geared towards a more reactive response rather than using preventative measures. Preventative measures, such as improving water, sanitation, and healthcare facilities as well as encouraging communities to adopt more hygienic behavior, are key to preventing the spread of cholera.
And, for an effective long-term approach, the prevention and control of cholera also requires a coordinated multi-disciplinary approach that examines activities both within and outside the health sector.
A Synergetic Approach: Looking Beyond the Health Sector for Solutions
National and international organizations, such as the WHO, FAO, and CDC, are now looking at ways to approach human health through a more holistic lens, looking at inextricable connections among the environment, animal health, and human health through approaches such as “One Health.” One Health is the integrative effort of multiple disciplines working locally, nationally, and globally to attain optimal health for people, animals, and the environment. The phrase is new, but the One Health concept has existed for many centuries.
The current One Health initiative was created in response to the H1N1, Avian influenza, and Ebola outbreaks from the early 2000’s. At the 2007 International Ministerial Conference on Avian and Pandemic Influenza, 111 countries and 29 international organizations demonstrated their support to develop the One Health movement. Currently, nations such as Uganda and Rwanda are beginning to integrate One Health approaches into their national strategic plans.
By using One Health’s collaborative approach, countries can strategically identify multiple factors that affect the spread of cholera as well as solutions that might not be obvious initially. It is well documented that cholera is often linked to poor environmental conditions and scarcity in clean water. With One Health, countries can consider solutions that might not present themselves through a health-only lens. For example, clean water generation is key to preventing the spread of cholera, and studies reveal that high water quality, increased water flow, and water availability correlate with forest cover and healthy wetlands, which trap and filter out pollutants and also recharge groundwater points. With One Health, governments can explore long term strategic solutions that include supporting a healthy environment, leading to better human health outcomes and lessened disease burden.
There is little doubt that health impacts arising from the changing climate are bound to occur with more frequency and severity in coming years, and it is imperative that we plan for these globally. It is not enough to react to and treat diseases, such as cholera, as they occur because these are only temporary solutions. Instead, we must look at strategically planning health initiatives based on a multi-sectoral collaboration and a One Health lens – only then can we find solutions to tackle our changing environment and our changing health.
Blog posts on the Chemonics blog represent the views of the authors and do not necessarily represent the views of Chemonics.