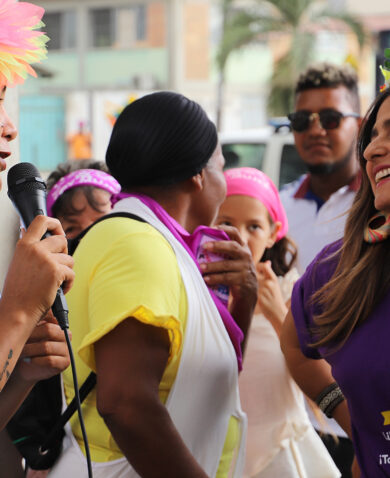Empowering Health Workers to #BeBoldforChange
March 10, 2017 | 3 Minute ReadOn International Women’s Day, HRH2030 reflected on how to empower health workers to #BeBoldforChange by ensuring provision of gender-equitable health services to women and girls.
This blog post originally appeared on the HRH2030 program website.
When we think about gender and human resources for health (HRH), we typically think about the challenges women face to fully participate in the workforce. Are women able to enter pre-service education institutions — and complete their courses of study — at the same rate as their male counterparts? Is there a pay gap for men and women performing the same work? But, what about the challenges that women and girls face when seeking gender-equitable health services? On International Women’s Day earlier this week, we recognized the challenges that women and men in the health workforce face, but we also recognized the power that all health workers wield to be agents of change. With that, we pose the question:
How can we empower health workers themselves to #BeBoldforChange?
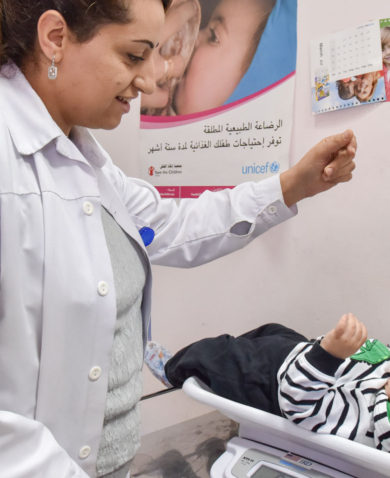
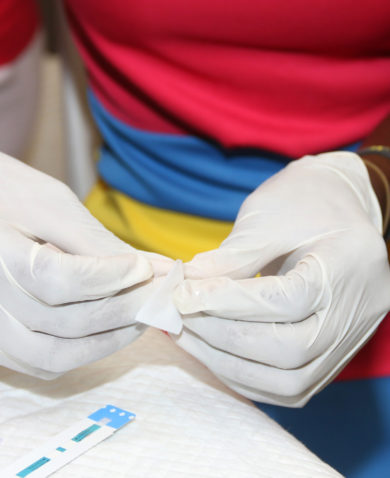
In large part, frontline health workers determine the experiences of clients coming to health facilities. A midwife could be critical of a pregnant teenager and treat her dismissively, or she could treat her patient respectfully as a soon-to-be mother coming to receive information during an antenatal care visit. A woman visiting a clinic to receive an HIV test might turn around when she sees she has to register and wait in front of two male nurses she knows from her community, or she might stay when offered a more private and comfortable place to wait for her HIV test from a provider of the same gender. A young woman visits a clinic to receive family planning information. Her counselor never asks about gender-based violence (GBV), so she never speaks up about the abuse she endures at home; or her counselor routinely asks her about GBV, so she has the opportunity to tell a trained professional.
Providers are not blank slates. Like any human being, they bring their biases and personal judgments to workplace interactions. Unfortunately, women’s ability to access a full range of care and information is affected by these biases. In some contexts, adult women are treated as minors who require permission or decisions by others in order to make health choices. Likewise, providers have a tendency to connect options with their personal judgment of women’s morality. For example, research in Rwanda found that health workers interpreted the recommendation to involve men in HIV-testing at the first antenatal care visit as a mandatory requirement, which ostracized single mothers and actually seemed to dissuade women from completing all four recommended visits. If we can improve providers’ ability to distinguish gender bias and provide regular, evidence-based, and accurate information, we can increase women’s access to quality care.
Through increasing gender competence, health workers can #BeBoldforChange and achieve more positive health outcomes. As countries make progress in health workforce development, a critical missing piece is that health workers at all levels lack information about gender and how to appropriately incorporate gender- equitable approaches into the provision of care.
For example, in Nicaragua, the USAID-funded Applying Science to Strengthen and Improve Systems (ASSIST) Project identified a knowledge gap in teachers at pre-service education institutions. A baseline survey uncovered that teaching staff at universities for physicians and nurses did not clearly understand the concepts of sex and gender, or the magnitude of gender-based violence. There was total ignorance of the legal framework for gender equality and the prevention of GBV; moreover, teachers did not know how to discuss or address issues in the university community. In response, ASSIST designed a training on gender and GBV to improve the understanding of gender among newly trained nurses and physicians. On average, teachers’ knowledge and attitudes following the training improved 22 percent.
To further this work, the USAID-funded HRH2030 program is defining what it means to be a gender-competent health care provider. The program is doing this by comparing the definition of gender competence for inclusion with existing competencies. For example, do existing competencies require a provider to routinely ask about GBV and/or provide full information on a range of health options? Or, does a lack of defined gender competencies lead to providers making assumptions of clients’ needs based on gender? This comparison will show the difference between the ideal of a gender-competent health professional against the actual gender competence of providers. Using the resulting gaps, HRH2030 can inform improvement of curricula at the pre-service education level to strengthen gender competence as a health provider skill. Understanding what it means to be gender-competent and applying gender awareness to the provision of care will enable pre-service institutions to incorporate gender into competency-based education. It will also give supervisors a framework to actively coach and mentor providers in gender competency and will give professional associations the ability to integrate gender awareness into licensing and certification. Most importantly, it will empower health workers to #BeBoldforChange, forging a more inclusive and gender-equal world.